Role of ADH, Renin-Angiotensin and Aldosterone in Osmoregulation
1. ADH (Anti-diuretic Hormone)
- Antidiuretic hormone (ADH) has the primary role in osmoregulation by controlling the amount of urine formation.
- ADH is also known as Vasopressin
- Body maintain water and electrolytes concentration at a relatively constant level by the mechanism of osmoregulation. Hormone are important signaling molecules that control the regulatory process.
- ADH is synthesized in hypothalamus and secreted by posterior pituitary gland.
- When blood become more concentrated in certain situation such as- Too little amount of water intake, Excessive loss of water by sweating or Consumption of large amount of salt. These conditions are responsible for raised in plasma solute concentration (rise in negative osmotic pressure) ie. Decrease in blood volume.
- The osmo-receptor of Hypothalmus detect increase in plasma solute concentration and signal posterior pituitary gland to release ADH.
- ADH travel to the kidney via the blood as chemical messengers.
- ADH regulates water reabsorption by increasing the permeability of distal convoluted tubules and collecting ducts to water by opening water channel. Water channel are protein, which is synthesized by Golgi complex.
- Binding of ADH on specific cell surface receptor present in DCT and collecting ducts bring water channel to the surface of membrane. Through water channel, water enter from glomerular filtrate to the blood capillary, so that the volume of urine become less and hypertonic. This phenomenon is known as Anti-diuresis.
- When intake of water is high, the process reversed. Release of ADH is inhibited, so the wall of DCT and collecting duct become impermeable to water causing large volume and hypotonic urine production. The phenomenon is known as Diuresis.
- Function: ADH increases the reabsorption of water by the distal tubule and collecting duct
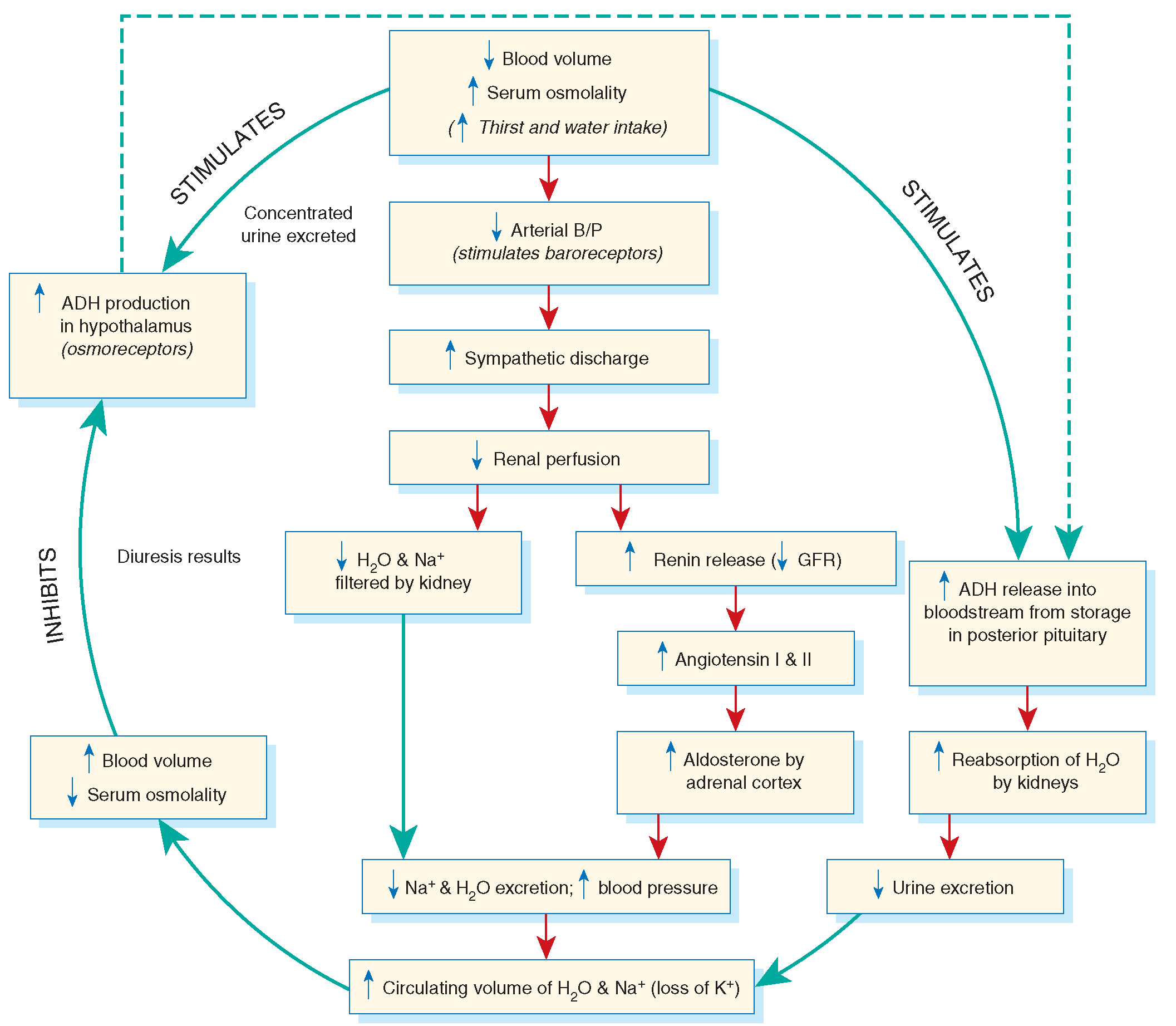
Feedback regulation of ADH
Hypothalamus control ADH production by negative feedback mechanism
- stimulates ADH synthesis, if osmotic concentration of extracellular fluid is high; urine-concentrated
- reduces ADH synthesis, if osmotic concentration of extra cellular fluid and plasma falls; urine-dilutes
Deficiencies of ADH
- Deficiency of ADH or non-functional ADH production causes a clinical disease called Diabetes insipidus. The clinical sign is output of large volume of urine frequently which is due to inadequately reabsorption of water by DCT and the collecting duct. Thrust is the symptoms of the disease.
2. Renin-Angiotensin system
- Renin is an enzyme secreted by juxtaglomerular apparatus that catalyze the conversion of angiotensinogen into active angiotensin hormone.
- When Na+ level decrease in blood. It causes decreased in blood volume and interstitial fluid level because less amount of water enter the blood by osmosis. This result in decreased blood pressure and trigger RAAS.
- The decrease in blood pressure stimulates the group of sensory cells present in the area where the renal tubule (DCT) links up with the afferent and efferent arterioles known as Juxtaglomerular apparatus.
- The cells of the juxtaglomerular apparatus release the enzyme Renin. Renin converts angiotensinogen into angiotensin I.
- Angiotensin converting enzyme (ACE) then converts angiotensin I into angiotensin-II;a peptide hormone that is the active form.
Function:
- Angiotensin-II Stimulates sodium reabsorption by the proximal convoluted tubules. Retaining Na+, raises the osmotic pressure of the blood and reduces water loss from renal tubules
- Raises blood pressure directly by constricting blood vessels
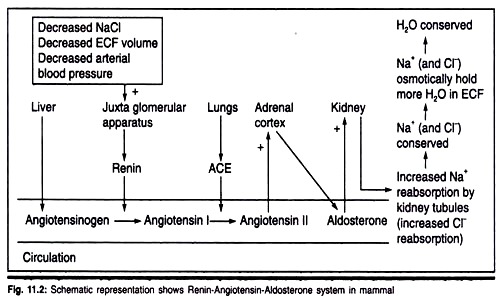
3. Aldosterone hormone
- Aldosterone is a hormone secreted by the outer cortical layer of the adrenal gland.
- Angiotensin II Increases the synthesis and release of aldosterone.
- Aldosterone stimulate Na-K pump, so that more Na+ from the filtrate is reabsorbed by the epithelial cells of the collecting ducts.
- Aldosterone also stimulate sodium absorption from gut and decrease loss of sodium from sweat. Thus, level of Na+ increases in blood, this in turn causes more water absorption raising the volume and blood pressure
Function: Maintain constant plasma Na+ level and also help water reabsorption
References
- https://en.wikipedia.org/wiki/Renin%E2%80%93angiotensin_system
- http://www.tutorvista.com/content/biology/biology-iv/excretion/role-kidney-osmoregulation.php
- http://study.com/academy/lesson/renin-angiotensin-aldosterone-system-raas-pathway-functions-terms.html
- http://www.people.vcu.edu/~elmiles/hormones/KidneyHormones_print.html
- http://www.nbs.csudh.edu/chemistry/faculty/nsturm/CHE452/22_RenAngioAldoANP18.htm
- https://www.boundless.com/biology/textbooks/boundless-biology-textbook/osmotic-regulation-and-the-excretory-system-41/hormonal-control-of-osmoregulatory-functions-232/other-hormonal-controls-for-osmoregulation-868-12115/
- https://bio.libretexts.org/TextMaps/Map%3A_General_Biology_(OpenStax)/7%3A_Animal_Structure_and_Function/41%3A_Osmotic_Regulation_and_Excretion/41.5%3A_Hormonal_Control_of_Osmoregulatory_Functions
